The Scrutiny of a Deadly Virus, Nipah

26-year-old Sabith was a fair-minded youth by all means. He was a plumber by profession and was very fond of animals and children. But it took Nipah only a matter of time to snatch his dreams and life from him. We are talking about Sabith, the first victim of the deadly Nipah virus. Around May 3rd, a feverish Sabith was taken to the hospital. His condition worsened all of a sudden and on May 5, when he began to loose consciousness, his family shifted him to the Kozhikode Medical College. But later in the night, Sabith passed away.
Soon after Sabith’s demise, the incidents took another toll. It was on May 17th. Around 2 AM, Mohammed Salih’s parents rushed him to Baby Memorial Hospital, Kozhikode. He was vomiting, had a high fever, and was in a mentally agitated state. A 28-year-old architect from Perambra, Kerala, was the brother of Sabith, who had already succumbed to similar symptoms just a week ago. The critical care physician of the hospital Dr. A.S Anoop Kumar understood it in a blink. All the symptoms led to encephalitis, which means the inflammation of brain tissue. Even after trying hard, doctors couldn’t stabilize him. It was obvious that something was not right when at around 9 AM the hospital’s neurologists came to examine him.
He was getting all the medical care he could possibly get, but his condition continued to rapidly deteriorate. His heartbeat was hitting high at 180 beats per minute, and his blood pressure had also risen up. He didn’t show any reflex since his limbs were limp. Dr. C. Jayakrishnan, one of the neurologists who treated him and his team started to rule out different causes of encephalitis since the symptoms were unlike any encephalitis cases that the team had ever seen. About 12 days ago, his brother passed away of similar symptoms, and their father and aunt had contracted the infection too. So they dismissed the chance of having Japanese encephalitis, since it wouldn’t affect more than one person in a household.
It was not rabies either. If the family had been exposed to a common pet, they would have fallen sick at the same time. But in this case, Salih had fallen sick days after his brother was infected. So they removed Rabies from the list. So, no illness matched with his symptoms. That’s how they concluded that the case they are dealing with might be new in the state and would require thorough work-through.
The Diagnosis
Dr. G. Arun Kumar is the head of the virology department in Manipal Centre for Virus Research (MCVR). Salih’s samples were dispatched to MCVR for further scrutiny. Dr. Arun Kumar has a history of investigating several mystery outbreaks before. Previously he dealt with Scrub Typhus in Uttar Pradesh’s Gorakhpur and encephalitis-like syndrome in Odisha’s Malkangiri district. He has been working on a surveillance project which aims at testing patients across 10 states over 40 pathogens. Since MCVR had upgraded one of their labs to Biosafety level, Dr. Arun Kumar got a chance to expand his research. When Salih’s samples arrived there, Dr. Arunkumar doubted something he was trained to detect before, Nipah virus.
In 2017, MCVR team was trained by United States’ Centers for Disease Control and Prevention to test for the Nipah virus, making MCVR the second laboratory in India to test Nipah other than Pune’s National Institute of Virology (NIV). Nipah has a history of high mortality. Two Reasons attracted Dr. Arun Kumar to test Nipah. The first one is both of the states of Tripura and Assam were across the border of Bangladesh and potential geographies for Nipah were covered under his surveillance project. Also, Nipah was considered to be a Bioterrorism Agent. Dr. Arun Kumar knew that among all the pathogens that cause encephalitis only one pathogen match with Salih’s symptoms and that was ‘Nipah’. Dr. Arun Kumar took the samples of Salih for a test called Real-Time Polymerase Chain Reaction (RT-PCR), which detects viral genetic material and discovered the pathogen to be Nipah.
The Nipah Wave
During its first outbreak in Malaysia in 1998, the virus infected and killed about 105 people. In Bangladesh, out of 196 cases infected, around 150 died which made the mortality rate 77%. The pathogen which acted in Malaysia and Bangladesh were different in the mode of operation. In Bangladesh, the virus was transmitted from one person to another through respiratory droplets. But this feature was absent in the pathogen which infected in Malaysia. Nipah was different in the mortality rates too. While the mortality rate in Bangladesh was 77%, till now out of 19 affected, Nipah claimed the lives of 17, which makes the mortality rate 89%.
But how did the state managed to control the spread of infection? The answer is, through collective effort. In 2001, when Nipah made a comeback in Siliguri, the first infection was reported in Siliguri district Hospital and the patient spread the illness to 9 others. Two other patients admitted to two other nursing homes, spread the infection to 34 others. It was like a chain. The majority of victims were hospital staffs. In Kerala, during Sabith’s stay in Hospital, nurses attended him, and dozens of neighbors came to look him up. This close contact has led to seven new cases in Perambra Taluk Hospital and 10 in Kozhikode Medical College. Yet, compared to the previous outbreaks the number of newly confirmed cases in Kerala has slowed down after the first wave of Infection. Thanks to the quick response of Kerala government and the effort of health officials, at least we were able to decrease the number of affected. According to 2005 International Health regulations, India is obliged to report to WHO, once an epidemic outbreak. But since a country has to be undoubtedly sure about their findings, MCVR sent Sabith’s family’s samples to Pune Virology Institute. But Dr.Arun Kumar knew it would take time and they’ve got no time to spare. So he informed Baby Memorial Hospital team to isolate the suspected patients since they were dealing with a deadly virus. By the time Salih got admitted to hospital, Kozhikode district medical officer, V. Jayashree, had learned about the virus and assigned a team to visit the infected house in Perambra. They first collected mosquitoes and fogged the area thinking that mosquitoes were the disease hosts. It was on May 20th Dr. Arun Kumar shared the final results. Same morning an officer, who was trained in Ebola outbreak protocols, instructed the State’s doctors to adopt the infection-control measures like isolating patients, using surgical masks and decontaminating surfaces. Nipah mainly spreads through respiratory droplets and sicker patients secrete the virus more. But the state can be considered Nipah free only after 42 days of the outbreak since the Nipah virus can incubate in the body for up to 21 days.
Who are the real suspects?
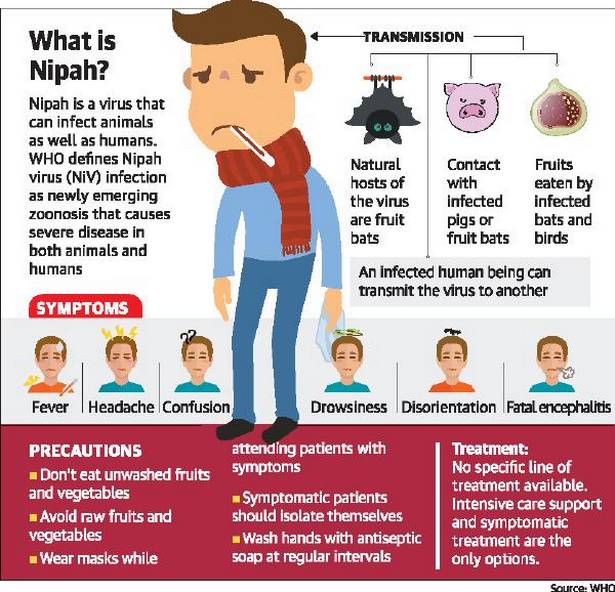
The natural hosts of Nipah virus are fruit bats also known as flying foxes. In the previous outbreaks in Malaysia and Bangladesh, fruit bats were the carriers of the virus. But in this case, how Sabith contracted the virus still remains a question. Since the previous carriers were fruit bats, a team from Pune NIV are currently camping in Kozhikode, to collect the samples from fruit bats. Nipah virus exists in bats only for a brief period of time. So it’ll be a difficult task for the team to collect samples and conduct necessary tests. According to American Journal of Tropical Hygiene and Medicine, virologists tried to isolate pathogens from collected samples of fruit bats in Malaysia and Bangladesh only a few days after the outbreak, but they were unable to isolate the pathogens in most case. According to Jonathan Epstein, an epidemiologist with the U.S.-based EcoHealth Alliance and an author of the study, “Unless your timing is good, and you are collecting samples close to when the first case was exposed, your chances diminish,”.
Here, In Kerala, the only thing to hope for was that the mammals may still carry antibodies to the Nipah virus, which remain for longer. But even if they do, it isn’t clear if NIV will test for antibodies, in addition to the viral genes.
Not only that but also since its monsoon season in Kerala, it’ll be difficult to collect the bat droppings and urine from the ground. Also, the Indian flying foxes may weigh over a kilogram and have a wingspan of up to five feet making it tough for entrapment and sample collection.
But even if the fruit bats are found to be the carriers, how could’ve Sabith come in contact with them? Maybe while cleaning the well where the investigating team found a dead bat which later tested negative for the Nipah virus. Or Is it through half bitten fruits? The question remains a mystery.
Source : http://www.thehindu.com/news/national/kerala/anatomy-of-an-outbreak-how-kerala-handled-the-nipah-virus-outbreak/article24060538.ece
Image credits: The Hindu
Neuroglia Health Private Limited.